INTRODUCTION
The morbidity
of the Urinary Tract infection (UTI) in the infancy is very high resulting in
permanent renal damage causing hypertension or end stage renal failure. It is
known that the UTI is more frequent in boys in the first three months of life.
The sex distribution is reported to be 5:1 with male predominance.1
Neonates present with poor weight gain, hypothermia, colour changes of the
skin, abnormal crying, irritability, abdominal distension, malodorous urine,
vomiting, diarrhea, rash, jaundice and hepatospleenomegaly.2 By
preschool age, the sex ratio is reversed, with majority of the urinary tract
infections occurring in the females. Recurrence is common and occurs in
approximately 18% of the male and 26% of female infants.3 Fever
remains a more common presentation in the neonates, infants and younger
children whereas older children present with other symptoms.4 Eighty
(80%) of the infants with culture proven UTI present with fever.5 Dysuria
can also be the main symptom of the UTI in younger children and infants.6
They present as irritability during micturition. Dysuria may be associated with
enuresis and foul smelling turbid urine.7 Urinalysis was also
recommended in infants presenting with jaundice.8 Along with other
sign and symptoms failure to thrive is also noted in the children with
recurrent UTI and may be the only positive physical finding.9 Paediatric
investigators have identified the risk factors associated with an increased
risk of UTI in children less than 2 years of age. They include temperature
higher than 39°C, fever longer than two days, white race, age less than one
year and no other obvious source of fever. The presence of two or more of the
above risk factors yielded a sensitivity of >99% and specificity of 71% for
the detection of UTI in this age group.10
The purpose of this study was to analyze
the clinical presentation of UTI in infants and children presenting at Ayub
Teaching Hospital with an idea to expedite diagnosis and thus reduce the
morbidity associated with it.
MATERIAL AND METHODS
All patients admitted
in the Paediatric wards of Ayub Teaching Hospital, Abbottabad were included in
the study. Non probability (convenience) sampling technique was applied. Age,
sex, weight and address were recorded. A detailed history was taken with
special emphasis on the antecedent history of UTI and other diseases like
diabetes mellitus, history of fever, dysuria, vomiting, urine colour, urinary
stream, abdominal pain and discharge urethra. All the patients were thoroughly
examined especially looking for their height, weight, failure to thrive,
temperature, jaundice, abdominal tenderness, palpable kidneys, and palpable
urinary bladder, any other visible external deformity related to urinary tract
and rachitic rosary. One hundred patients with diagnosed UTI were included in
the study.
RESULTS
Majority of patients (46%) belonged to the
age group 13 to 60 months. Fever
was most common presentation. The detail is given in table-1 and Figure-1.
DISCUSSION
UTI is a significant problem in Abbottabad District
and Northern areas of
Table-1: Clinical presentations of UTI in children(n=100)
|
Presentation |
Present |
Absent |
|
Fever |
92% |
8% |
|
Dysuria |
68% |
32% |
|
Failure to thrive |
31% |
69% |
|
Weak urinary stream |
20% |
80% |
|
Discharge urethra |
15% |
85% |
|
Previous episode of UTI |
28% |
72% |
|
Altered colour of urine |
12% |
88% |
|
Vomiting |
26% |
74% |
![]()
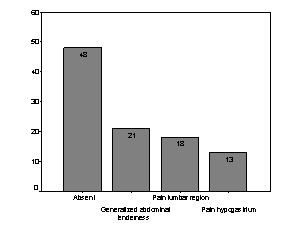
Figure-1: Abdominal tenderness in the patients with UTI
The number of the patients was
less in the neonatal period and the cases increased with the increasing age and
declined after the thirteen years of age till fifteen years. It is also
reported by many studies.1,12 Fever was the
most common symptom in the 100 enrolled cases. 92% of the patients had history
of fever. 20.3% of the children presented with fever in another study.15
The difference in the study was due to the fact that fever alone, as the only
prese-nting symptom was considered by them. However other studies also indicate
the high association between the fever and urinary infection.4,5,10,16,17
Failure
to thrive was common (31%) in my study as compared to the studies from
different countries.14,15 No data is available on failure to thrive
and its association with UTI in
Underlying
malnutrition with added infection and poor intake has been blamed for it.18
Jaundice is considered to be a common presenting symptom in neonates and
infants with UTI.19 Only one patient presented with jaundice during
the neonatal period and was found to be due to the Rh incompatibility. The
difference could be due to the small sample size in my study and there is also
evidence of decrease in cases of jaundice due to UTI.20
Dysuria
is a common presentation in older children (4% to 60.8%), but it can also be a
presenting symptom in the infants.15,21 Most of the observations were
beyond 48 months of age. The difference seen in various studies is due to the
difference in the patients age groups. Dysuria was reported in 4% neonates,21
and upto 60.8% cases15 in patients beyond neonatal period.
There was a poor relationship between the urine colour and the urine culture
positive UTI. A significant number (88%) of children presented with normal
colour of urine and no change in the smell of the urine. Similar results were
reported by a study conducted in St. Mary’s Hospital, Portsmouth.7
A
strong relationship was observed between UTI and combination of dysuria with
weak urinary stream. In this study all the patients presenting with both
dysuria and weak urinary stream had positive urine cultures. A significant
percentage of children (28%) presented with recurrent urinary infection. In
females, poor compliance and follow-up were identified as major problems. In
males, the urinary tract abnormalities were also contributory.
Failure
to thrive was another underlying cause for recurrent urinary tract infections
in both the sexes. In one report the recurrence of UTI after first attack is
approximately 30% and can be as high as 75% in children after second or third
episode of UTI.7 Recurrent episodes are the main reason for the
development of vesicoureteral reflux and eventually leading to end stage renal
failure.18
Pain
abdomen is also a non specific finding in patients having UTI, 48% of our
patients did not have any pain. Others presented with generalized abdominal
pain, lumber tenderness and hypogastric pain in descending order of frequency.
It is also reported by others with similar findings.14
There
were other associated findings in patients with UTI, like urethral discharge
and palpable urinary bladder. A small number of patients presented with lower
UTI like symptoms: 11% with palpable urinary bladder and 15% with urethral
discharge. It is comparable to other studies, where children were identified
with lower urinary tract symptoms (9.5%) as having UTI.15
REFERENCES
1.
Langley JM, Hanakowski M, Leblanc JC. Unique epidemiology of nasocomial
urinary tract infection in children. Am J Infect Control 2001; 29: 94–8.
2.
Falcao MC, Leone CR, D’Andrea RA, Berardi R, Ono NA, Vaz FA. Urinary
tract infections in full-term newborn infants: value of urine culture by bag
specimen collection. Rev Hosp Clin Fac Med Sao Paulo1999;54: 91–6.
3.
Barnett BJ, Stephens DS. Urinary
tract infection: an over view. Am J Med Sci 1997; 314:245-49
4.
Kaushal RK, Sumeet B, Sharma VK, Sood A, Goyal A. Urinary tract
infection among children presenting with fever.
5.
Shaw KN, Shortliffe LMD. Urinary tract infection in the pediatric
patient. Pediatr Clin North Am 1999;46(6):1111-24
6.
Bagga A. consensus statement on management of urinary tract infections.
7.
Struthers S, Scanlon J, Parker K. Parental reporting of smelly urine and
urinary tract infection. Arch Dis Child 2003;88:250-52
8.
Garcia FJ, Negar AL. jaundice as an early sign of urinary tract
infection in infancy. Pediatrics 2002;109:846-51
9.
Bartkowski DP. Recognizing UTIs in infants and children. Postgrad Med.
2001;109(1):171-81
10.
11. Wammanda R.D., Ewa B.O. Urinary tract pathogens and their
sensitivity pattern in children. Annals of Tropical Pediatrics 2002;
22:197-198.
12. Arslan S, Caksen H, Rastgeldi L. use of urinary gram stain for the
detection of urinary tract infection in childhood. Yale Journal of Biology and
Medicine 2002;75:73-8.
13. Mehr SS, Powell CV, Curtis N.
cephalosporin resistant urinary tract infections in young children. J Paediatr
Child Health 2004;40(1-2):48-52
14. Gallager SA, Hemphill RR. Urinary Tract Infections: Epidemiology,
Detection, and Evaluation. [Cited on 2003]. Available from: www.ahcpub.com
15. Saleh SI, Tuhmaz MM, Sarkhouh
MY. urinary tract infection in children in Al-jahra area,
16. Gorelick MH, Shaw KN.
Screening test for UTI in children: A Meta analysis. Pediatrics 1999;104(5):e54
17.
18. Elder JS. Urinary
tract infection. Behrman RE, Kliegman RM, Jenson HB, editors. Nelson Textbook
of Pediatrics. 17th ed.
19. Crain EF, Gershel JC. Urinary
tract infections in febrile infants younger than 8 weeks of age. Pediatrics
1990;86:363-67
20. Newman TB,
Bernzweig JA, Takayama JI, Finch SA, Wasserman RC, Pantell RH. Urine testing
and urinary tract infectoin in febrile infants sen in office settings: The
Pediatric Research In Office Settings’ Febrile Infants Study. Arch Pediatr
Adolesc Med. 2002;156:44-54
21. Biyikli NK, Alpay
H, Ozek E, Akman I, Bilgen H. Neonatal
urinary tract infections: Analysis of the patients and recurrences. Pedtr Int
2004; 46:21-25.