J Ayub Med Coll Abbottabad 2003;15(1)
RADIAL KERATOTOMY: EFFECTS OF CORNEAL THICKNESS ON FINAL OUTCOME
Naseer Raja, Muhammad Khizar Niazi, Sobia Karamat
Department of Ophthalmology, Military Hospital, Rawalpindi, Pakistan.
Background: Corneal thickness may contribute in the final outcome of radial keratotomy operation for the correction of myopia. We present our study on ninety-nine consecutive eyes with a mean follow-up of one year. Methods: Ninety-nine eyes with preoperative/uncorrected Myopia between 2.5–6.0D and a mean age of 29.2 (±7) years underwent radial keratotomy between January 1999–December 2001 in the Department of Ophthalmology, Military Hospital, Rawalpindi. The eyes were divided based on their corneal thickness into group-A (51 eyes), with a pachymeter reading of 500–540 µm, and Group-B (48 eyes), with a pachymeter reading of 541–580 µm. The comparison between the Postoperative visual acuity of two groups was made at the end of study after one years` follow up. Results: Forty-five eyes (88.23%) in Group-A improved to an uncorrected acuity of 20/20 as compared to forty eyes (83.33%) in Group-B (p>0.05). Hyperopic shift occurred in two eyes (3.92%) in Group-A, as compared to ten eyes (20.83%) of Group-B (p>0.05). Refraction showed that 94.11% cases of Group-A to be within 1 diopter of Emmetropia as compared to 93.75% cases in Group-B. Similarly, 98.03% cases of Group-A were within 2 diopters of Emmetropia as compared to 95.83% cases of Group-B. Glare and variation of vision in the initial four weeks were the most frequently reported complications in both groups. Conclusion: Thickness of cornea does not significantly affect the outcome of surgery in cases of low to moderate degrees of myopia.
KEYWORDS: Radial Keratotomy, Corneal Thickness, Myopia
INTRODUCTION
Radial keratotomy (RK) is a widely accepted surgical procedure to correct myopia. In the operation, sets of 4-12 evenly spaced radial incisions are made in the treated cornea, which extend from the boundary of a central optical clear zone of specified diameter to the outer periphery of the cornea1.
The intraocular pressure causes the weakened peripheral region of the cornea to bulge outward and flatten the central visual region by stretching it like a drumhead. The central flattening reduces the refractive power of the anterior corneal surface, and the focal point is shifted posteriorly to the surface of the retina producing corneal flattening after the operation2.
The effectiveness of this procedure depends on the surgeon's ability to select surgical variables that lead to the desired reduction in the refractive power3. Many preoperative and preoperative variables affect the outcome of the surgery such as refractive state of the patient, axial length of the cornea, age of the patient, or systemic disease, depth of incision, as well as extension of the incision3-5 etc. So far, no local study has been documented regarding the effect of corneal thickness on results of surgery.
We conducted our study to find out the effect of corneal thickness on results of radial keratotomy.
MATERIAL AND METHODS
The study was conducted in the Department of Ophthalmology, Military Hospital, Rawalpindi from Jan 1999 to Dec 2001. Ninety-nine cases were included in the study. The subjects were between 21–40 years of age, had stable preop refraction for at least two consecutive years, myopia between 2–6 Diopters, and corneal pachymetry between 500–580 µm. Patients with history of Diabetes, Collagen vascular disorders, ocular trauma or previous eye surgery, examination finding of a conjuctival, corneal or lenticular pathology, having eyes with high IOP, or irregular astigmatism were excluded from the study. Blood complete picture, ESR, fasting blood glucose were done to rule out associated diseases.
All cases were examined thoroughly under slit lamp and cycloplegic refraction was done to confirm the findings and correction required. Preoperative thirty-spot screening Pachymetry was done and the central corneal thickness was taken as the standard for thee study. All of these cases underwent an eight-incision radial keratotomy by a single surgeon (author) using the combined approach, with a double edged diamond Knife (Duckworth and Kent), done as an out door procedure.
Preoperatively 0.5% Proparacaine eye drops were used for the local anaesthesia. Intraoperative corneal pachymetry was done at 1.5 mm from the visual center, at the 3 mm central clear zone, and calibration and adjustment of Diamond knife was done accordingly. After applying the selected radial marker for several seconds, the knife was entered at the central corneal margin and a centrifugal radial incision was initiated, penetrating about 90–95% of corneal stroma, making a cut to 1 mm within the limbus. This procedure was repeated so that eight incisions were made.
Postoperatively the eyes were padded and Tab. Diclofenac Sodium six hourly, was given for pain. They were then seen on the following day and advised 0.1% Dexamethasone drops six hourly for the first week and then eight hourly for one week.
Follow-up was done at six weeks, two months, four months, sixth months and finally at one year of surgery. On the basis of pachymetry, the subjects were then divided into two groups. Group A comprised of fifty-one cases with a corneal pachymetry of 510–540 µm, whereas Group-B consisted of forty-eight cases with pachymetry of 541–580 µm. In each follow-up, the unaided visual acuity, hyperopic shift, under or overcorrection was noted by cycloplegic refraction with 1% Cyclopentolate eye drops.
Questions were specifically asked about the presence of glare, fluctuation of vision during the day, pain or photophobia and corneal examination was done to look for any signs of infection or wound gap. The significance of difference between the two groups regarding final unaided visual acuity and degree of hyperopic shift was determined at the end of study with χ2 test.
RESULTS
The mean age of the patients was 29.2 (±7) years. Results of investigations are shown in Table-1.
Table-1: Mean results of investigations (n=99)
|
Tests (SI Units) |
Mean Results |
|
Blood ESR (mm fall at 1 hour) |
12±10 mm fall |
|
Blood Glucose Fasting (mmoles/l) |
4.8±3.0 mmole/l |
|
Blood Complete Picture |
Within Normal Range in 87% High Total Leucocytes in 08% Low Platelet Count in 05% |
The mean follow up time was twelve months. Forty-five eyes (88.23%) of Group-A attained a final unaided vision of 20/20 in the operated eye, whereas this vision was achieved in forty eyes (83.33%) of Group-B (p>0.05). Refraction showed that 94.11% cases of Group-A to be within 1 diopter of Emmetropia as compared to 93.75% cases in Group-B. Similarly, 98.03% cases of Group-A were within 2 diopters of Emmetropia as compared to 95.83% cases of Group-B. These results are summarized in the Table-2.
Table-2: Comparative results at the end of study (n=99)
|
Groups (Corneal Thickness) |
Unaided Visual Acuity |
Spectacle Correction |
Hyperopic Shift |
|||
|
20/20 (6/6) |
20/25 (6/9) or Worse |
Within 1D Of Emmetropia |
Within 2D Of Emmetropia |
Present |
Absent |
|
|
A=51 (510–540) |
45 |
6 |
48 |
50 |
2 |
49 |
|
B=48 (541–580) |
40 |
8 |
45 |
46 |
10 |
38 |
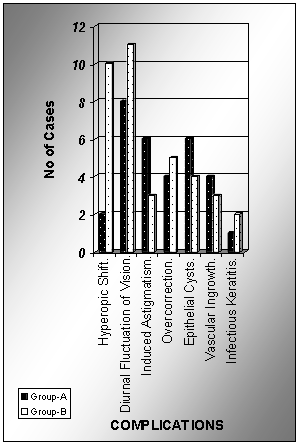
Complications of the procedure were few and did not adversely affect the visual outcome of any case. The most common was glare especially at night, seen in eighteen eyes (18.18%) that gradually cleared itself with the passage of time. Hyperopic shift occurred in two cases of Group-A (3.92%), as compared to ten cases (20.83 %) of Group-B (p>0.05). The frequency of complications is given in Figure-1.
Figure-1: Frequency of complications after surgery (n=99)
DISCUSSION
Modern radial keratotomy technique is based on multiple radial incisions of 85%–95% stromal depth that terminate 1 mm or more inside the limbus6. It was adapted for use by the ophthalmic professional community in 19787-9, and the multicentre, PERK study (Prospective evaluation of Radial Keratotomy) done over a ten-year period in USA has contributed much to the current understanding of the predictability and stability of the refractive result after radial keratotomy10. It is a safe and effective method to correct low myopia up to -6.00 diopters (D)11, the technique offers various advantages: clinical experience of more than 15 years, fast visual rehabilitation, minimal discomfort postoperatively, and low cost and technical requirements12-16. Nevertheless, the final refractive outcome could be variable from individual to individual due to difference in response to injury among the population, resulting in over corrections and under corrections in a certain percentage of patients17. Possible complications include glare and fluctuation of vision18, hyperopic shift, infectious keratitis, and endophthalmitis19. It neither weakens nor causes increased susceptibility of cornea to trauma than a normal eye20. The role of corneal thickness in the results of radial keratotomy was not mentioned earlier in the literature. We undertook our study with the same aim. Ninety-nine cases with low to moderate degrees of myopia (-1.5 to -6.0 D) were included in the study. The results were evaluated by comparing a patient’s refractive error and uncorrected vision before and after surgery. A comparison between our results and studies done abroad is given Table-3.
As shown in the results, the outcome of surgery between the two groups was not statistically significant. Regarding the complications of the procedure, when asked directly, all patients were satisfied with the result of their operation in general; eighteen patients complained of glare that gradually subsided with the passage of time. Patient satisfaction was high and 78% of the patients elected to undergo radial keratotomy in their fellow eye.
Table-3: A comparison of various studies on radial keratotomy
|
Study |
PERK study21 |
Arrowsmith and Marks22 |
Deitz and Sanders23,24 |
Our study |
|
Year of surgery |
1982-83 |
1980-81 |
1982-85 |
1999-2001 |
|
Follow up time |
3 years |
5 years |
1 year |
1 year |
|
No of eyes |
435 |
122 |
972 |
99 |
|
No of incisions |
8-16 |
8 |
8-16 |
8 |
|
Knife Blade |
Diamond (single edge) |
Steel |
Diamond (double edged) |
Diamond (double edged) |
|
Central clear cornea |
3.0-4.0 mm |
3.0-5.0 mm |
2.7-6.0 mm |
3.0 |
|
Over-corrected 1.0D |
16% |
33% |
12% |
9% |
|
Under- corrected 1.0 D |
18% |
13% |
12% |
10% |
|
Uncorrected VA>6/12 |
76% |
76% |
88% |
98% |
REFERENCES
1. Wanga JQ, Zenga YJ, Lib XY. Influence of some operational variables on the radial keratotomy operation. Br J Ophthalmol 2000; 84: 651-653.
2. George O, Waring I. Refractive keratotomy for myopia. Verlag 1985; 911-917.
3. Waring GO. Development of refractive keratotomy in the United States, 1978-1990 In: Waring GO: Refractive Keratotomy for Myopia and Astigmatism. St Louis, MO: MosbyYear Book Inc; 1992: 237-258.
4. Sawelson H, Marks R. Five year results of refractive keratotomy. Refract Corneal Surg 1989; 5: 133-144.
5. El-Maghraby A, Salah T, Polit F, Ballew MC, Deluca MC, Raanan MG. Efficacy and safety of excimer laser photorefractive keratectomy and radial kratotomy for bilateral myopia. J Cataract Refract Surg 1996; 22: 51-58.
6. Fernando Hm. ed. Refractive disorders. In: Fraunfelder FT, Roy FH. Current ocular therapy. Philadelphia. WB Saunders Company 2000; 31: 591.
7. Bores LD, Myers M, Cowden J. Radial keratotomy – An analysis of the American experience. Ann Ophthalmol. 1981; 13: 941-948.
8. Rowsey JJ, Balyeat HD, Rabinovitch B. Predicting the results of radial keratotomy. Ophthalmology 1983; 90: 642-654.
9. Werblin TP, Stafford GM. The Casebeer system for predictable keratorefrative surgery. One-year evaluation of 205 consecutive eyes. Ophthalmology 1993; 100: 1095-1102.
10. Waring GO, Lynn MJ, Nizam A. PERK Study Group. Results of the Prospective Evaluation of Radial Keratotomy (PERK) Study five years after surgery. Ophthalmology 1991; 98:1164-1176.
11. Krumeich JH, Daniel J, Gast R. The suction Bridge for Radial Keratotomy may avoid late hyperopic shift. J Refract Surg 1997;13: 367-373.
12. Leaming DV. Practice styles and preferences of ASCRS members: 1993 survey. J Cataract Refract Surg 1994; 20: 459-467.
13. Waring GO, Lynn MJ, McDonnell PJ, and the PERK Study Group. Results of the Prospective Evaluation of Radial Keratotomy (PERK) study 10 years after surgery. Arch Ophthalmol 1994; 112: 1298-1308.
14. Binder PS, Waring GO, Arrowsmith PN, Wang CL. Traumatic rupture of the cornea after radial keratotomy. Arch Ophthalmol 1988; 106: 1584-1590.
15. Ellis W. Radial Keratotomy and Astigmatism Surgery. Irvine, CA: Keith C. Terry and Associates; 1986: 117-130.
16. Waring GO, Lynn MJ, Culbertson W. PERK Study Group. Three year results of the Prospective Evaluation of Radial Keratotomy (PERK) study. Ophthalmology 1987; 94: 1339-1354.
17. Raja N, Niazi MK, Ahmed N. Evaluation of hundred cases of radial keratotomy. J Pak Armed Forces Med 2002; 52: 57-61.
18. Neumann AC, Osher RH, Fenzl RE. Radial keratotomy: a comprehensive evaluation. Doc Ophthalmol 1984; 56(3): 275-301.
19. Choi DM, Thompson Jr RW, Price Jr FW. Incisional refractive surgery. Curr Opin Ophthalmol 2002; 13(4): 237-241.
20. Lindstorm RL. Comparison of RK and PRK. In: Pallikaris IG, Siganos DS, eds. Lasik. New Jersey: Slack Incorporated, 1998;17: 189-194.
21. Waring GO, Laibson P, Lindstorm R. Changes in refraction, keratometry, and visual acuity during the first year after radial keratotomy in the PERK study. Invest Ophthalmol Vis Sci 1985; 26: 202-205.
22. Arrowsmith PN, Marks RG. Visual, refractive, and keratometric results of radial keratotomy: A year follow-up. Arch Ophthalmol 1987: 5: 76-80.
23. Sanders DR, Deitz MR, Gallagher D. Factors affecting the predictability of radial keratotomy. Ophthalmology 1985; 92: 1237-1243.
24. Deitz MR, Sanders DR, Marks RG. Radial keratotomy: An overview of the Kansas City study. Ophthalmology 1984; 91: 467-477.
Address for Correspondence:
Col. Dr. Naseer Raja, Department of Ophthalmology, Military Hospital, Rawalpindi, Pakistan. Email: khizar_aleem@yahoo.com