INTRODUCTION
EUS is now considered the standard of care for staging of oesophageal, gastric, pancreatic and rectal cancers. The primary advantage of EUS over other forms of imaging, such as CT and MRI, is its unique ability to accurately stage mucosal depth of invasion of tumours. This often upstages lesions extending beyond the serosa, and thus prevents unnecessary surgery.1,2 With the advent of linear EUS, a number of interventions have become possible. Gastroenterologists can now perform EUS-guided FNA and core biopsies of lymph nodes and other masses in the mediastinum and abdomen.3 Accessible liver metastases can also be biopsied through the oesophageal or gastric wall. Indeterminate pancreatic tumours, submucosal tumours and large gastric folds mimicking gastric varices or otherwise causing diagnostic confusion, can all be biopsied using linear EUS. Other therapeutic manoeuvres, such as EUS-guided coeliac plexus block4,5 and transgastric endoscopic pseudocyst drainage6,7, are also possible. Current modalities available to obtain tissue from mediastinal masses include CT-guided FNA or core biopsy, mediastinoscopy, video-assisted thoracic surgery (VATS) and EUS-FNA. Recently, transbronchial needle biopsy of mediastinal nodes has also been described.8 Each procedure has its own risks and benefits. EUS-FNA is safe, well-tolerated and avoids exposure to radiation and anaesthesia associated with other methods.
CASE HISTORY
A 54-year-old male smoker with
COPD presented with a six month history of increasing hoarseness and a productive
cough. A chest radiograph revealed a mediastinal mass
with left hilar lymphadenopathy.
Following the procedure, the patient was observed for one hour to exclude immediate complications, before being allowed home. Based on the EUS-FNA findings, the patient was deemed inoperable and was referred for palliative radiation therapy.
DISCUSSION
In linear echoendosonography, the ultrasound beam travels in a plane parallel to the shaft of the endoscope, allowing tracking of instruments extending from the working channel of the endoscope, so that EUS-guided FNA and core biopsies of lymph nodes and other masses in the mediastinum and abdomen3 can be performed. Liver metastases, pancreatic tumours, submucosal tumours and large gastric folds mimicking gastric varices can all be biopsied. EUS-guided coeliac plexus block4,5 and transgastric pancreatic pseudocyst drainage6,7, are also possible. EUS- guided FNA is very safe9, with only occasional infectious complications being reported. Apart from the initial costs of equipment and training, consumable costs are low and a re-usable FNA needle is available.
EUS provides the most accurate assessment available for the staging of oesophageal cancer. It has been shown to be superior to CT in this respect1 as well as for staging of gastric carcinoma.10 EUS-guided FNA of mediastinal masses is now a standard procedure in many countries.9 Several studies support the use of EUS-guided FNA for diagnosing pancreatic masses.11-16
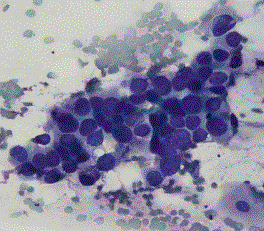
Figure-1: FNA showing small clusters of atypical
epithelial cells, with cellular crowding and nuclear overlapping, high nuclear-cytoplasmic ratio and hyperchromatic
nuclei, with occasional small nucleoli. The cytoplasm is pale to clear. The
cytological features are consistent with non-small cell lung cancer.
CONCLUSION
EUS-guided aspiration of mediastinal masses is a safe and well-tolerated procedure.
This case serves to highlight the need for expanding facilities in selected
hospitals to allow physicians to train in and perform such advanced techniques.
Cancer is an increasingly common diagnosis in
REFERENCES
1.
Botet JF, Lightdale
CJ, Zauber G, Gerdes H, Urmacher C, Brennan MF. Preoperative staging of oesophageal
cancer: comparison of endoscopic US and dynamic CT.
Radiology 1991;81:419-25.
2.
Rosch T, Lorenz R, Zenker K. Local staging and assessment of resectability in carcinoma of the oesophagus, stomach and
duodenum by endoscopic ultrasonography.
Gastrointest Endosc 1992;38:460-7.
3.
Suits J, Frazee R, Erickson RA. Endoscopic
ultrasound and fine needle aspiration for the evaluation of pancreatic masses.
Arch Surg 1999;134(6):639-42;
4.
Wiersema MJ, Wiersema
LM. Endosonography-guided celiac plexus neurolysis. Gastrointestinal Endoscopy
1996;44(6):656-62.
5.
Gress F, Schmitt C, Sherman S, Ikenberry S, Lehman G. A prospective randomized comparison
of endoscopic ultrasound- and computed
tomography-guided celiac plexus block for managing chronic pancreatitis
pain. Am J Gastroenterol 1999;94(4):900-5.
6.
Wiersema MJ. Endosonography-guided
cystoduodenostomy with a therapeutic ultrasound
endoscope. Gastrointest Endosc
1996;44:616-7.
7.
Giovannini M, Bernardini
D, Seitz JF. Cystogastrostomy entirely performed
under endosonography guidance for pancreatic pseudocyst: results in six patients. Gastrointestinal Endoscopy 1998;48(2):200-3.
8.
Hermens FH, Van Engelenburg TC, Visser
FJ, Thunnissen FB, Termeer
R, Janssen JP. Diagnostic yield of transbronchial
histology needle aspiration in patients with mediastinal
lymph node enlargement. Respiration. 2003;70(6):631-5.
9.
Janssen J, Johanns W,
Greiner L. Clinical value of endoscopic
ultrasound-guided transoesophageal fine needle
puncture of mediastinal lesions. Dtsch
Med Wochenschr 1998;123(47):1402-9.
10. Snady H. The role of endoscopic ultrasonography in diagnosis, staging and outcomes of
gastrointestinal disease. Gastroenterologist 1994;10:91-110.
11. Gress FG, Hawes RH, Savides TJ, Ikenbery SO, Lehman GA. Endoscopic
ultrasound-guided fine-needle aspiration biopsy using linear array and radial
scanning endosono-graphy. Gastrointestinal Endoscopy 1997;45(3):243-50.
12. Wiersema MJ, Vilmann P, Giovannini
M, Chang KJ, Wierseman LM. Endosonography
guided fine-needle aspiration biopsy: diagnostic accuracy and complication
assessment. Gastroenterology 1997;112:(4)1087-95.
13. Giovannini M, Seitz JF, Monges G, Perrier H, Rabbia I. Fine needle aspiration cytology guided by endoscopic ultrasonography
results in 141 patients. Endoscopy 1995;27(2):171-7.
14. Chang KJ,
Albers CG, Erickson RA, Butler JA, Wuerker RB, Lin F.
Endoscopic ultrasound-guided fine needle aspiration
of pancreatic carcinoma. Am J Gastro 1994;89(2):263-6.
15. Chang KJ,
Nguyen P, Erickson RA, Durbin TE, Katz KD. The clinical utility of endoscopic ultrasound-guided fine-needle aspiration in the
diagnosis and staging of pancreatic carcinoma. Gastrointestinal Endoscopy 1997;45(5): 387-93.
16. Faigel DO, Ginsberg GG, Bentz JS,