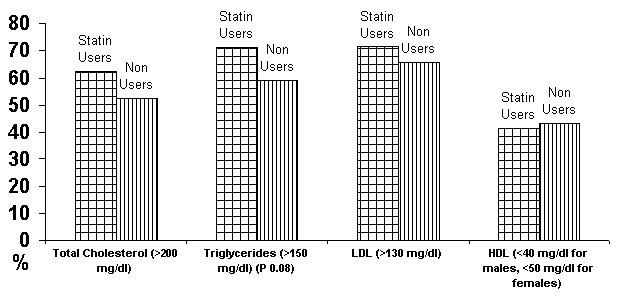
Figure-1:
Prevalence of lipid abnormalities according to Statin
use
FREQUENCY OF
STATIN USE IN TYPE 2 DIABETICS HAVING MACROVASCULAR DISEASE- AT A
Abdul Basit,
M. Zafar Iqbal Hydrie, Rubina Hakeem,* M. Yakoob Ahmedani,
Qamar Masood
Baqai Institute of Diabetology
and Endocrinology,
Background: During the last two decades with the
introduction of statins large reductions in
cholesterol concentrations were easily and safely achievable and this led to
studies that demonstrated benefits of statin use. But
only fewer than one fourth of adults with coronary
heart disease were receiving lipid-lowering drugs in a cross sectional health
survey done in
Keywords: Statin Users, Frequency,
Lipid profile, Type 2 Diabetes,
INTRODUCTION
Diabetic dyslipidemias are related to cardiovascular disorders and
also associated with the macrovascular complications
of diabetes. Macrovascular complications are among
the chief causes of major morbidity and mortality in people with diabetes 1-2.
Diabetes has 3-5 times higher absolute risk of coronary heart disease (CHD)
death at each level of blood cholesterol than non-diabetic subjects 3.
In the
last 20 years studies have indicated that smoking cessation, beta blockers,
anti-platelet agents, ACE-inhibitors and lipid lowering agents, each reduce the
risk of vascular events to a moderate but important degree 4-7. With
the introduction of statins large reductions in
cholesterol concentrations were easily and safely achievable and this finding
led to a series of studies that demonstrated benefits in selected populations.
Several
large studies such as 4S8, CARE9 and LIPID10
have provided evidence for effectiveness of lipid-lowering drugs in macrovascular disorders; and have proven that lowering Low
Density Lipoproteins (LDL) with statins reduces the
risk of CHD mortality and morbidity in high risk patients by a quarter to half.
The CHD risk was higher among the subjects with diabetes than those without it,
hence the absolute benefits of statins appears to be
larger in diabetics. The ATP-III report by the National Cholesterol Education
Program (NCEP) lists high LDL levels to be the major cause of CHD and diabetes
is taken as CHD risk equivalent 11. United Kingdom Prospective
Diabetes Study (UKPDS) has also shown direct association of CHD risk with LDL
levels among 3000 type 2 diabetic subjects and inverse association with HDL
Cholesterol 12.
Heart
Protection Study (HPS) has also clearly shown that lowering lipid levels with a
statin is of value in much broader populations than
currently realized and all patients with vascular disease or having CHD risk
would benefit from statins including those who were
poorly represented in other studies such as elderly (>75 years of age),
women, having LDL < 96 mg/dl, diabetics with no CHD and patients having
stroke or peripheral vascular disease 13.
Thus it
is universally recommended that statins should be
prescribed to all patients with coronary heart disease 14. Patients
with myocardial infarction (MI) are recommended to use statins
if their total cholesterol was > 180 mg/dl and patients with angina
should use statins if total cholesterol >
200 mg/dl 15.
Though
prescription of statins has increased in recent
years, it is still well below the recommended level in the treatment of
patients with coronary disease in
The purpose of
this study was to assess the type 2 diabetics with macrovascular
disease attending a tertiary care unit in
MATERIAL AND METHODS
Baqai Institute of Diabetology
and Endocrinology (BIDE) is a tertiary care hospital providing� specialist care to the diabetic population. ince its inception the institute maintains computerized
records of diabetic patients. For this study computerized records of the first
visit of all type 2 diabetic subjects older than 18 years of age to the
outpatient department of Baqai Institute of Diabetology and Endocrinology from September 1996 to
December 2001 was analyzed for their anthropometric and biochemical
characteristics. The information to be retrieved included computer code, age,
sex, occupation, place of residence, marital status, family history, smoking,
year of diagnosis of diabetes and medications already being taken. Therefore,
minimal confidentiality or ethical issues were involved. Furthermore names were
not disclosed anywhere and the researchers used only the computer code for
identification purposes.
Out of the total 2152 patients 502 subjects having any
macrovascular disease were identified and frequency
of statin use by these patients was studied.
Glycemic control was
assessed by fasting plasma glucose and HbA1c.
Venous plasma
glucose was estimated by GOD-PAP Method16. HbA1c was
assessed by DiaSTAT Hemoglobin A1c
Program, Bio-Rad17. HbA1c, was used
as the basic indicator of glycemic control. Values of
< 7%, 7 - 8.5% and > 8.5% indicated good, fair or poor control
respectively18. Where HbA1c
values were not available, fasting plasma glucose values were used to determine
glycemic control. FPG <126, 126-144, and >144
were taken as good, fair and poor control respectively18.
Total
cholesterol and high density lipoproteins were estimated by CHOD-PAP method
while triglycerides was estimated by GPO-PAP method and low density
lipoproteins values were calculated 19. Values of total
cholesterol� > 200 mg/dl,
triglycerides > 150 mg/dl, low density lipoproteins� > 130 mg/dl, high density lipoproteins
< 40 mg/dl for males and < 50 mg/dl for females were taken as abnormal 20.
The OPD
medical officer using a mercury sphygmomanometer measured blood pressure once.
Hypertension was defined as B.P >130/85 mmHg or isolated systolic &
diastolic blood pressure of greater than 130 & 85 mmHg respectively 22.
��������������� Patients with history of
Ischemic Heart Disease as evident by ECG changes or symptoms deemed sufficient
by the physician to be suggestive of angina or MI were termed as sufferers of
angina and MI. Those suffering from any macrovascular
and Myocardial infarction were labeled in the group of Myocardial infarction.
��������������� Patients with history of stroke
evident by signs & symptoms and physical examination as assessed by the
physician was termed as suffering from stroke. Those if suffering from angina
and stroke were labeled in the group of angina.
��������������� Peripheral Vascular Disease
(PVD) was inferred from absent dorsalis pedis or posterior tibial pulses
with/without a history of intermittent claudication.
Those if suffering from angina and PVD were labeled in group of angina. Those
if suffering from PVD and stroke were labeled in the group of stroke.
Data was entered
and analyzed on SPSS 7.5. ANOVA was used for estimating statistical
significance of differences in means of continuous variables. Chi-square test
was used to assess statistical significance of difference in categorical
variables.
RESULTS
Out of total
diabetics, 502 subjects (23.3 %) were found to have any of the macrovascular symptoms (MI,
24.9%; angina, 56.7%; stroke, 15.7%; PVD, 2.6%). All available
bio-chemical parameters were analyzed and mean values are given in table-1.
Only 16.5% of the patients were using any statins.
Though the difference was not statistically significant the use was slightly
higher among males (17.5%) as compared to females (15.6%) (Table-2). Among
older subjects (>60 years of age) 18.6% were using statins
whereas in those less than 60 years the use of statins
was around 15%. This difference was also statistically non significant. In
terms of socioeconomic status use of statins was
slightly higher among businessmen and professionals (20% of all businessmen and
professionals)) as compared to skilled workers (15.7% of all skilled workers)
and housewives (15.6% of all housewives). In relation to vascular disease the
use of statins was most frequent among the angina
sufferers (20%), followed by those who had MI (16.9%), followed by stroke
sufferers (10%) while none of the peripheral vascular disease sufferers were
using statins (Table-3).
Table 1: Characteristics of the Sample
|
|
Male |
Female |
|
|
Mean + SD |
Mean + SD |
|
Age (years) |
57.5 + 10.2 |
55.9 + 9.7 |
|
Weight (Kgs) |
70.0 + 11.1 |
63.2 + 12.4 |
|
Height (metre) |
1.70 + 0.1 |
1.50 + 0.1 |
|
Body Mass Index (Kg/m2) |
25.3 + 3.5 |
27.1 + 5.0 |
|
Systolic Blood Pressure (mmHg) |
131.6 + 22.4 |
140.8 + 24.6 |
|
Diastolic Blood Pressure (mmHg) |
81.4 + 11.8 |
82.1 + 13.0 |
|
Cholesterol (mg/dl) |
197.2 + 47.8 |
206.5 + 45.8 |
|
Triglycerides (mg/dl) |
191.3 + 131.6 |
192.9 + 103.9 |
|
Low Density Lipoproteins (mg/dl) |
122.6 + 42.7 |
131.4 + 47.4 |
|
High Density Lipoproteins (mg/dl) |
37.7 + 9.0 |
37.9 + 11.0 |
|
Fasting Plasma Glucose (mg/dl) |
190.8 + 80.1 |
199.6 + 86.2 |
|
Random Plasma Glucose (mg/dl) |
256.0 + 92.4 |
262.5 + 105.0 |
|
HbA1c (%) |
8.7 + 2.3 |
9.2 + 2.3 |
Table 2: Statin use according to sex of Subjects
|
|
Statin Use |
|
|
|
Yes |
No |
|
Male�����
(n=252) |
44(17.5% ) |
208(82.5% ) |
|
Female�
(n=250) |
39(15.6%) |
211(84.4%) |
|
Total����� (n=502) |
83(16.5% ) |
419(83.5%) |
Table 3: Statin Use according to Macrovascular
disease of patients
|
|
Statin Use |
|
|
|
Yes |
No |
|
Angina (n=285) |
55(20.0%) |
230(80.0%) |
|
MI (n=125) |
20(16.9%) |
105(83.1%) |
|
Stroke (n=79) |
8(10.0%) |
71(90.0%) |
|
PVD (n=13) |
0(0.0%) |
13(100.0%) |
The
users of statins had higher values for triglycerides,
total cholesterol and LDL-C and lower mean values for HDL-C (figure 1).
The
results of this study shows a trend which has also been reported by other
researchers i.e under prescription of statins 23-24.
Only one fourth of
diabetic subjects with macrovascular disease were
taking statins for their lipid control. As the
duration of treatment for which statins had been prescribed
is not known, comments on the effect of use of statins
could not be given. The presence of higher proportion of subjects with diabetic
dyslipidemia in the statins
user group could be either due to the short period since commencement of
medication when they presented at BIDE or that they were under-dosed.
Though the
differences in the characteristics of the users and non-users did not reach
statistical significance the results of this study indicates that males,
relatively more affluent, older diabetics, those having angina and having
elevated triglycerides are more likely to get treated by statins.
Although the subjects presenting at BIDE are from a relatively narrow range of
socioeconomic status, housewives seem to be less likely to be started on statin. This trend of females not been started on statins has also been seen in other studies 24-26.
The Health Survey
for England and the British Regional Heart Study suggested that most older men
with CHD are not receiving lipid lowering drug treatment while in our study the
elderly diabetics with CHD were proportionally more on statin
treatment; probably as younger subjects were put on diet & exercise and not
considered for statins as a first line therapy by the
physicians 27.
It is surprising
that subjects with angina were more on statins as
compared to MI a reverse trend as seen in studies elsewhere. This highlights
the fact that subjects with MI were not given statins
as a part of therapy irrespective of lipid levels; perhaps having normal lipid
levels post MI been a reason for their not been started on statins.
Angina patients have a high absolute risk of acute coronary events and silent
MI in diabetics advocates for earlier treatment with statins
24-25.
In subjects with
type 2 diabetes blood triglycerides tend to be raised and HDL levels reduced
even with good metabolic control while LDL levels tend to be similar to those
seen in the general population. This has contributed to the belief that LDL is
of little relevance to the risk of CHD in diabetics and thus most people with
diabetes do not receive lipid lowering drugs despite their increased risk.
The statin user group in our study had markedly higher mean
values for triglycerides, total cholesterol & LDL and slightly lower value
of HDL. It is suggested that either the subjects were recently prescribed statins or higher doses of the drugs are required in these
patients to achieve target lipid levels; both of which could not be verified in
this study. By retrieving and analyzing data from a larger and more
heterogeneous group of subjects validity of these trends could be
verified.�
For the current
analysis information about previous physicians was not available so any trends
in the use of statins by various physicians could not
be explored. However despite the clear efficacy of statin
use it seems likely that physicians may vary in their knowledge, attitudes and
practices regarding the use of statins.
The
very low statin prescribing rate in CHD subjects is a
cause for concern especially as type 2 diabetic subjects has high morbidity and
mortality11. Thus there is a need to review the treatment of all
diabetic patients with CHD and make sure that patients are receiving the
benefits of starting treatment as early as possible.
Barriers to a more
wide spread use of statins may include fears about
the cost resulting in non-affordability as well as clinical practices. Since
80% of CHD occurs in developing countries it should be a priority to make
latest recommendations such as ATP III Report accessible to the physicians14.
Physicians are aware about the potential gains from the currently available
preventive strategies and it is hoped that enough studies have been done to
convince physicians that statins should be prescribed
for the vast majority (if not all) diabetic patients with CHD in both primary
and secondary care.
In conclusion the
results of this study verify the low prescribing rates of statins
in our community setting. In view of possible detrimental impact of this trend,
further studies are needed to identify the factors leading to low use of statins in type 2 diabetic subjects with macrovascular symptoms to ensure that patients receive this
treatment which will lead to clinical and public health benefits.

Figure-1:
Prevalence of lipid abnormalities according to Statin
use
ACKNOWLEDGMENT
We
acknowledge the co-operation of PharmEvo
REFERENCES
1.
Garcia MJ, McNamra PM, Gordon T. Morbidity
and mortality in diabetics in the
2.
Panzram G.
Mortality and survival in type 2 (non-insulin-dependent) diabetes mellitus. Diabetologia 1987:30;123-31
3.
Stamler J, Vaccaro O, Neaton JD. for the
Multiple Risk Factor Intervention Trial Research Group. Diabetes, other risk
factors and 12-year cardiovascular mortality for men screened in the multiple
risk factor intervention trial. Diabetes Care1993;16:434-44.
4.
Pechacek TF, Asma S, Eriksen MP. Tobacco:
global burden and community solutions. In: Yusuf S,
Calms A Camm AJ, Fallen EL, Gersh
BJ, eds. Evidence based cardiology.
5.
Yusuf S, Peto R, Lewis J, Collins R, Sleight P. Beta blockade during
and after myocardial infarction: an overview of the randomized trials. Prog Cardiovasc Dis 1985; 27:335-71.
6.
Antithrombotic Trialists Collaboration. Collaborative meta-analysis of
randomized trials of antiplatelet therapy for
prevention of death, myocardial infarction, and stroke in high risk patients.
BMJ 2002; 324: 71-86.
7.
Heart Outcomes Prevention Evaluation
Study Investigators. Effects of an Angiotensin-converting-enzyme
inhibitor, ramipril, on cardiovascular events in
high-risk patients. N Engl J Med 2000; 342:145-53.
8.
Scandinavian Simvastatin
Survival Study Group. Randomised trial of cholesterol
lowering in 4444 patients with coronary heart disease: the Scandinavian Simvastatin Survival Study (4S). Lancet 1994; 344:1383-57.
9.
Sacks PM, Pfeffer MA, Moye LA. The
effect of Pravastatin on coronary events after
myocardial infarction in patients with average cholesterol levels. N Engl J Med 1996; 336: 1001-09.
10.
The Long-term Intervention with Pravastatin in Ischemic Disease (LIPID) Study Group.
Prevention of cardiovascular events and death with pravastain
in patients with coronary heart disease and a broad range of initial
cholesterol levels. N Engl J Med 1998; 344:1383-99.
11.
Executive Summary of the Third
Report of the National Cholesterol Education Program (NCEP) Expert Panel on
Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult
Treatment Panel III). JAMA. 2001;285: 2486-2497.
12.
13.
MRC/BHF Heart Protection Study
Collaborative Group. MRC/BHF heart protection study of cholesterol-lowering
therapy and of antioxidant vitamin supplementation in a wide range of patients
at increased risk of coronary heart disease death: early safety and efficacy
experience. Eur Heart J 1999; 20:725-41.
14.
Yusuf S.
Commentary. Two decades of progress in preventing vascular disease. Lancet
2002; July 6;360:2-3.
15. Wood D, Durrington P, Mcinnes
P. Joint British recommendations on prevention of coronary heart disease in
clinical practice. Heart 1998; 80(suppl 2): S1-29.
16.
GOD-PAP
enzymatic colorimetric test. Trinder,P., Ann. Clin. Biochem., 6:24 (1969).
17. NGSP Steering Committee.�
Implementation of the National Glycohemoglobin
Standardization Program (NGSP). Diabetes 46(Suppl 1),
151A. 1997.
18. Alberti G.� A desktop guide to Type 2 diabetes mellitus.
European Diabetes Policy Group 1998-1999 International Diabetes Federation
European Region.� Exp.Clin.Endocrinol.Diabetes
1999; 107:390-420.
19. European Atherosclerosis Society.�
Strategies for the prevention of coronary heart disease: a policy
statement of the European Atherosclerosis Society.� Eur Heart J 1987;
8:77-88.
20.
NCEP.� Executive Summary of The Third Report of The
National Cholesterol Education Program (NCEP) Expert Panel on Detection,
Evaluation, And Treatment of High Blood Cholesterol In Adults (Adult Treatment
Panel III).� Jama
2001;� 285:2486-2497.
21.
World Health Organization, Regional
Office for the Western Pacific, International Association for the Study of
Obesity. International Obesity Task Force. The Asia-Pacific perspective:
redefining obesity and its treatment.
22.
NIH-NHLBI (National
23.
Reid FDA, Cook DG, Whincup PH. Use of statins in the secondary prevention of coronary heart
disease: is treatment equitable? Heart 2002; 88:15-19.
24.
Primatesta P, Poulter NR. Lipid concentrations and the use of lipid
lowering drugs: evidence from a national cross sectional survey. BMJ 2000;
321:1322-5.
25.
Anon. Key health statistics from
general practice 1998. Series M86, no 2.
26.
Hippisley-Cox J,
Pringle M, Crown N. Sex inequalities in ischaemic
heart disease in general practice: cross-sectional survey. BMJ 2001; 322:832-4.
27.
Whincup PH, Emberson JR, Lennon L. Low
prevalence of lipid lowering drug use in older men with established coronary
heart disease. Heart 2002; 88: 25-29.
Dr�
M. Zafar Iqbal Hydrie, Baqai Institute of Diabetology
and Endocrinology,
Email: bideresearch@hotmail.com
�