INTRODUCTION
Urinary tract can be defined by the presence of
significant quantity of bacteria in the urine along with signs and symptoms of
infection.1 Urinary tract infection (UTI) is an important cause of
bacteremia due to gram negative organisms. Prompt diagnosis and management of
UTI can reduce the incidence of morbidity and life threatening bacteraemia.2
Approximately 3-5% of the girls and 1% of the boys acquire a UTI. 3
UTI can lead to renal scars and if undiagnosed leads to permanent renal damage
causing hypertension or end stage renal disease. The diagnosis of UTI is
difficult in the neonatal period because the signs and symptoms are
non-specific in this age group. The incidence in the neonates is 0.01-1% and
can also be as high as 10% in low birth weight and preterm babies.4
Every child with a proven UTI deserves investigation after first attack.
However care must be taken not to expose the child to excessive investigations.5
Diagnostic workup should be modified to recognize any condition that leads to
stasis of the urine in the bladder. Renal calculi, obstructive uropathy
(posterior urethral valves), vesicoureteral reflux, and voiding disorders can
lead to urinary stasis and may predispose to the development of recurrent UTI
and complications.6
The pattern of
organisms has so far not been studied at Ayub Teaching Hospital. This study was
done to determine the different types of organisms and their respective
frequencies causing urinary tract infection in admitted patients at Paediatric
units of Ayub Teaching Hospital, Abbottabad in order to improve the management
of the patients.
MATERIAL AND METHODS
One Hundred patients of diagnosed urinary tract infection ages 0-15
years admitted in Ayub Teaching Hospital Abbottabad were included in the study
using non probability (convenience) sampling technique. A detailed history was
taken and complete clinical examination was carried out for each case of
urinary tract infection. Every patient
had urine microscopy, X-ray of kidneys and urinary bladder, urinary colony
count and urine culture investigations. The diagnosis of urinary tract infection
was based on microscopic finding of more than 5 white blood cells per high
power field on urine microscopy and a colony count of 105/ ml of
single pathogen. In Neonates the urine was collected through supra pubic
approach. In uncooperative and moribund patients the urine was also collected
through the supra pubic puncture or urinary catheterization. In infants and older
children the urine was collected in urine collecting bag or sterilized
container, after washing the genital region with soap and water. Mid stream,
clean catch, early morning specimens were collected in a sterilized container. All the antibiotics were discontinued
72 hours before sending the urine for culture and sensitivity. Urine sample was
delivered to the laboratory within 1 hour of collection. In case of delay the
urine samples was kept at 4oC and analyzed within 6 hours of the
collection. The urine samples
were cultured in 5% sheep blood agar and MacConkey’s media. Inoculation was
done with the help of a 0.001ml caliber loop. All the sample plates were incubated for 48
hrs at 37oC in 5-10% carbon dioxide for anaerobic growth. Bacterial
identification was done by hand lens and standard biochemical tests. Where
multiple growths were obtained the culture was repeated again before accepting
the results. The details of each patient were recorded in a proforma.
RESULTS
The results of this study are shown in table-1 and figure-1.
Table-1: Organisms isolated in
different age groups expressed in percentages
|
Age Group |
Escherichia coli |
Klebsiella
pneumoniae |
Proteus |
Staphylococci |
Pseudomonas |
Total |
|
0-12 months |
3 (4.2%) |
1 (7.6%) |
Nil (0%) |
2 (50%) |
Nil (0%) |
6 (6%) |
|
13-60 months |
33 (46.5%) |
6 (46.2%) |
7 (63.6%) |
1 (25%) |
Nil (0%) |
46 (46%) |
|
61- 120 months |
28 (39.4%) |
5 (38.6%) |
3 (27.3%) |
1 (25%) |
1 (100%) |
39 (39%) |
|
121-180 months |
7 (9.9%) |
1 (7.6%) |
1 (9.1%) |
0 (%) |
Nil (0%) |
9 (9%) |
|
Total |
71 (71%) |
13 (13%) |
11 (11%) |
4 (4%) |
1 (1%) |
100 (100%) |
Figure No. 1 Pathogens isolated on urine
culture.
DISCUSSION
Most of the
infections were observed in the female patients with an overall male to female
ratio of 1:2.3. Males out numbered females during the first year of life with a
ratio of 1.5:1; this is in full agreement with other studies.7-11
Female preponderance has been observed after one year of age (3.5:1ratio).
Several studies in children above one year of age till fifteen years reported
female predominance, with a variable ratio ranging from 6:1 to 1.33:1,
depending upon the different sample size, and difference in age groups being
studied.11-15
Majority
of patients (46%) belonged to the 13 to 60 month age group and this coincides
with studies from Zaire12, Turkey13, United States15,
Australia16, Kuwait17, and Iran.18 This could
be because of the reason, as reported by other studies that this age group of
13-60 months is more susceptible to infections due to their toilet training
problems.9 The number of the patients was less in the neonatal
period and the cases increased with the increasing age and declined after the
thirteen years of age till fifteen years. It is also reported by many studies.11,
13
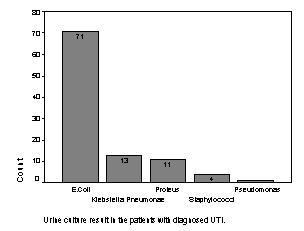 The organisms infecting the urinary tract in this study were
E.coli (71%), Klebsiella pneumoniae (13%), Proteus species (11%),
Staphylococcus (4%), Pseudomonas (1%) in their descending order of percentages.
These results are similar to many latest published articles.3,14,18 However, a few studies have indicated a lower
percentage of E.coli infections and a higher infection with Proteus and
Klebsiella species.4,13,19,20 On the other hand some have given a
higher percentage of E.coli infection as compared to other organisms.16,17
This could be explained on the basis of sampling technique and the gender
difference in different studies. Female predominance was observed with an
overall ratio of 1:2.3. It was in
concordance with other studies.3-5,13,14,17-22 During the first year
of life males were infected more. This was also reported by all other
researchers. 3-5,13,14,17-19 Proteus was isolated in the males (11%) only.
It was reported in many papers that Proteus mainly affects males with a high
incidence in them. In one study from Turkey Proteus was isolated in male
patients only.13 This has been explained on the ability of the
Proteus species to swarm the long urethra of the males and ascend to cause the
infection. Staphylococcus and Pseudomonas remain the least infecting organisms
(4% and 1% respectively). These results are consistent with other studies. The
urinary infections caused by Staphylococcus ranged from 0.7% to 8.5% in
different studies.4,13,14,17 Staphylococcus were identified in the
neonates and a diabetic patient, where as Pseudomonas was isolated in a
cerebral palsy child with marasmus.
The organisms infecting the urinary tract in this study were
E.coli (71%), Klebsiella pneumoniae (13%), Proteus species (11%),
Staphylococcus (4%), Pseudomonas (1%) in their descending order of percentages.
These results are similar to many latest published articles.3,14,18 However, a few studies have indicated a lower
percentage of E.coli infections and a higher infection with Proteus and
Klebsiella species.4,13,19,20 On the other hand some have given a
higher percentage of E.coli infection as compared to other organisms.16,17
This could be explained on the basis of sampling technique and the gender
difference in different studies. Female predominance was observed with an
overall ratio of 1:2.3. It was in
concordance with other studies.3-5,13,14,17-22 During the first year
of life males were infected more. This was also reported by all other
researchers. 3-5,13,14,17-19 Proteus was isolated in the males (11%) only.
It was reported in many papers that Proteus mainly affects males with a high
incidence in them. In one study from Turkey Proteus was isolated in male
patients only.13 This has been explained on the ability of the
Proteus species to swarm the long urethra of the males and ascend to cause the
infection. Staphylococcus and Pseudomonas remain the least infecting organisms
(4% and 1% respectively). These results are consistent with other studies. The
urinary infections caused by Staphylococcus ranged from 0.7% to 8.5% in
different studies.4,13,14,17 Staphylococcus were identified in the
neonates and a diabetic patient, where as Pseudomonas was isolated in a
cerebral palsy child with marasmus.
REFERENCES
1.
Zelikovic
I,
2.
Yousaf
M, Ahmad M, Khan HH, Yousaf N, Microorganisms causing urinary tract infection
and their anti microbial sensitivities. Pak Inter J Med Res 1993;32: 294-6.
3.
Elder
JS. Urinary tract infection. Behrman RE, Kliegman RM, Jenson HB, editors.
Nelson Textbook of Pediatrics. 17th ed.
4.
Biyikli
NK, Alpay H, Ozek E, Akman I, Bilgen H.
Neonatal urinary tract infections: Analysis of the patients and recurrences.
Pedtr Int 2004;46:21-5.
5.
Vohra
NA, Urinary tract infection in Children. Specialist 1992;8(4):63-7.
6.
Khaliq MA, Jehangir A, Khan SP, Aziz F.
Bacteriological study of urinary tract infection in healthy school going
children of Hazara division.
7.
Mobley
HL, Island MD, Massad G. Virulence determinants of Uropathogenic Escherichia
coli and Proteus mirabilis. Kidney Int Suppl 1994;47: S129-S131.
8.
Jakobsson
B, Esbjorner
E. Sverker H. Minimum Incidence and Diagnostic Rate of First
Urinary Tract Infection - Statistical Data Included.Pediatrics 1999;104(2):222-6.
9.
Gallager SA, Hemphill RR. Urinary Tract Infections: Epidemiology,
Detection, and Evaluation. [Cited on 2003]. Available from: www.ahcpub.com.
10.
Hellerstein S.
Urinary tract infection in children: why they occur and how to prevent them. Am
Fam Physician 1998; 46(2):2440-51.
11.
Langley JM,
Hanakowski M, Leblanc JC. Unique epidemiology of nasocomial urinary tract
infection in children. Am. J. Infect. Control 2001;29:94–8.
12.
Wammanda R.D., Ewa B.O. Urinary tract pathogens and their
sensitivity pattern in children. Annals of Tropical Pediatrics 2002;22:197-8.
13.
Arslan S, Caksen H, Rastgeldi L, Uner A, Oner AF, Odabas D.
Use of urinary gram stain for the detection of urinary tract infection in
childhood. Yale Journal of Biology and Medicine 2002;75:73-8.
14.
Waisman Y, Zerem E, Amir L, Mimouni M. The Validity of the
Uriscreen Test for Early Detection of Urinary Tract Infection in Children.
Pediatrics 1999;104(4):p. e41.
15.
Barnett BJ, Stephens DS. Urinary tract infection: an over
view. Am J Med Sci 1997;314:245-9
16.
Mehr SS, Powell
CV, Curtis N. Cephalosporin resistant urinary tract infections in young
children. J Paediatr Child Health 2004;40(1-2):48-52
17.
Saleh SI, Tuhmaz
MM, Sarkhouh MY, El-Ghawabi MA. Urinary tract infection in children in Al-jahra
area,
18.
Modarres S, Nassiri N. Bacterial etiologic agents of urinary
tract infection in children in the Islamic Republic of Iran.
19.
Falcao MC, Leone
CR, D’Andrea RA, Berardi R, Ono NA, Vaz FA. Urinary tract infections in
full-term newborn infants: value of urine culture by bag specimen collection.
Rev Hosp Clin Fac Med Sao Paulo1999;54: 91–6
20.
Acharya VN, Jadav
SK. Urinary tract infection: current status. J Postgrad Med 1980;26:95-8
21.
Sood S, Upadhyaya
P, Kapil A, Lodha R, Jain Y, Bagga A. An indigenously developed nitrite kit to
aid in the diagnosis of the urinary tract infection. Indian Pediatr 1999;
36:887-90
22.
Crain EF, Gershel
JC. Urinary tract infections in febrile infants younger than 8 weeks of age.
Pediatrics 1990; 86:363-7.